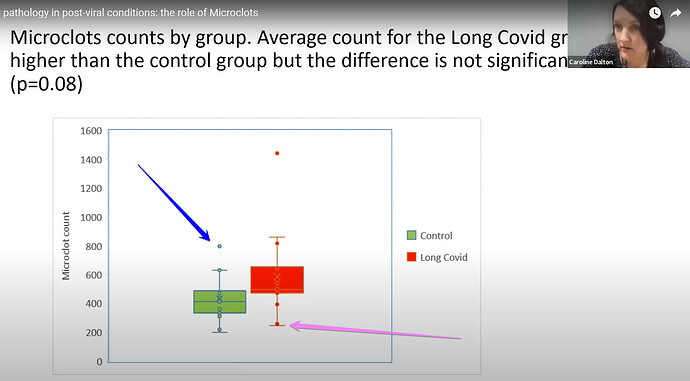
First of all, what you should know is that the ‘science’ from Pretorius, Kell, and their colleagues was not done in good faith.
#1
Version 1 of their preprint claimed that all 24 of 24 patients got better on triple anticoag.
Then version 2 of that preprint removes all of the clinical data. It calls for RCTs without mentioning any of the clinical data that they had.
Given all of the LC and MECFS patients that tried triple anticoag, it seems highly likely that the 100% response rate was fabricated.
#2
The authors have a history of saying things to get research funding. When they were researching T2DM, they said that microclots were important. When acute CVD was a hot research topic, they said that microclots were responsible for low oxygen levels in the blood. Then when they got into LC, they said that microclots were the cause of LC symptoms… even though they had already know that some healthy controls, T2DM, and acute CVD patients have abnormal levels of microclots without LC symptoms.
Douglas Kell maintains (and continually updates) an easy-to-understand summary of their current thinking on his website. A snapshot is here: https://web.archive.org/…/http://dbkgroup.org/longcovid/
The current version is here: http://dbkgroup.org/longcovid/
I have concerns about certain doctors and scientists because they could have figured it out like I did. Either they didn’t put in the work, they relied on others for information, or they don’t want to know.
DOES IT WORK?
A number of ME/CFS and Long C patients have already tried triple anticoag. The response rate definitely is not 100%. Usually with every therapy you will find that there are multiple people reporting success, so what we really want to know is the success rate and have some type of consistent definition of recovery (because everybody defines it differently).
With survey data, we can guess the success rate and have a consistent definition of recovery. However, I only have survey data on individual anticoag therapies. Clopidogrel may have a low response rate (like other top treatments) or it may do nothing in terms of helping people recover. Aspirin is like that too, but it’s more likely that aspirin doesn’t help people recover.
Clopidogrel/Plavix has a boxed warning because it is less effective in some patients (2-14%) because of their genes. Those people do not effectively metabolize the prodrug into the active drug.
Two #TeamClots members on Twitter have chronic illness. Asad Khan has Long COVID while Harriet Carroll has postvax. Neither are able to work normally despite Khan’s HELP apheresis and Carroll’s anticoag treatment.
“DETOX”
Some doctors may claim that your body is detoxing or Herxing when treatments are first given to you. This may be a dangerous idea because it would cause you to ignore signs that the treatment is hurting you. However, this idea does help the doctor retain patients and improve their profitability.
SCIENCE FROM ANIMAL EXPERIMENTS
Both LC patients vax injured patients are diagnosed with new-onset autoimmune conditions at very high rates. see the risk factors survey https://www.longhaulwiki.com/…/V%F0%9F%A5%95ccn_injury…
A number of blood thinning drugs have been tried in animal models of autoimmune disease. At ridiculously high dosages, clopidogrel can cause a benefit. (Note that many treatments that can cause benefit also demonstrate harm in other contexts. These treatments cut both ways.) The other prescription blood thinners aren’t helpful.
https://odysee.com/…/PAMPs-and-the-connection-between…
I haven’t seen evidence that detox effects are occurring. Rather, the science strongly suggests that the effective treatments are double edged swords. They will hurt some patients. If the drug is hurting you, you are not detoxing. You are simply being hurt by the drug.
I have concerns about the medical experimentation going too far, the lack of reliable data, and the quality of medical services being provided.