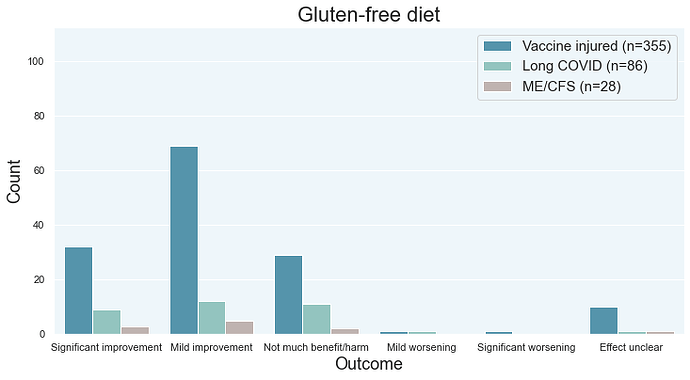
Key points:
![]() Very few people report adverse effects from a gluten-free diet.
Very few people report adverse effects from a gluten-free diet.
![]() This diet can provide rapid relief of symptoms for people who react to gluten.
This diet can provide rapid relief of symptoms for people who react to gluten.
![]() The chance of recovery may be low (or perhaps zero). Only 1.2% of surveyees reported being mostly recovered AND rated this diet as leading to significant improvement.
The chance of recovery may be low (or perhaps zero). Only 1.2% of surveyees reported being mostly recovered AND rated this diet as leading to significant improvement.
This diet probably won’t cure you. However, the safety of this intervention looks excellent compared to the other options out there.
Here are some conditions where gluten-free diets may help (or are known to help):
- Celiac disease, which is often undiagnosed.
- Non-celiac gluten sensitivity.
- Irritable bowel syndrome. The mechanism of action may be (mostly) unrelated to gluten.
- Autoimmune disease
Undiagnosed celiac disease and non-celiac gluten sensitivity
Some research suggests that celiac disease commonly goes undiagnosed. A 2003 study by Fasano et al. (DOI:10.1001/archinte.163.3.286) does a deep dive into the topic. It cites a survey of patients:
a recently published survey of 1612 patients with CD in the United States revealed that the average gap between the onset of symptoms and the time CD diagnosis was confirmed was 11 years
Survey data from the Risk Factors Survey shows that about 5% of long COVID and post-vax patients have a celiac diagnosis. See slide 9 (16/302 people). This 1-in-19 prevalence (of only diagnosed CD) is likely much higher than the general population as Fasano and colleagues estimate a prevalence of 1-in-133 (both diagnosed and undiagnosed) in the not-at-risk groups in the general population. However, I don’t know what the underdiagnosis rate is for chronic illness patients… it may not necessarily be >5 times that of the general population.
There are also a few people who would benefit from a gluten-free diet even though they do NOT have celiac disease. They do not test positive on the biopsy test even though gluten affects their symptoms. See the literature on non-celiac gluten sensitivity (NCGS), e.g. Nutrients | Free Full-Text | Non-Celiac Gluten Sensitivity: The New Frontier of Gluten Related Disorders
Leonard, Fasano and colleagues wrote a review paper on NCGS (DOI:10.1001/jama.2017.9730) where they estimate celiac disease to have a prevalence of 1%. They go on to say this about NCGS:
The frequency of nonceliac gluten sensitivity is unknown owing to the lack of validated biomarkers, but it is thought to be more common than celiac disease.
Leonard, Fasano and colleagues make some suggestions about diagnosing NCGS. While a blinded test would be nice, they suggest being pragmatic and recognizing that a blinded challenge is “not generally feasible in a clinical setting”. So, they suggest that the patient adhere and not adhere to a gluten-free diet and then looking at symptoms.
Until biomarkers are identified and validated, the diagnosis of nonceliac gluten sensitivity is confirmed in a research setting with a doubleblind crossover gluten challenge.49 In a clinical setting, clinicians may suggest a blinded gluten challenge during which a patient is given approximately 8 g of gluten (corresponding to approximately 2 slices of bread) or placebo for 1 week each, separated by a 1-week gluten-free washout period. Symptoms are monitored throughout the challenge.49A blinded challenge is not generally feasible in a clinical setting; therefore, for patients with fluctuating symptoms, symptomatic assessment of a patient adhering vs not adhering to a gluten-free diet for at least 1 week is suggested.49
Irritable Bowel Syndrome (IBS)
A department at Monash University has been studying IBS sufferers. First they ran double-blind controlled trials and found that patients were getting better on a gluten-free diet. They did more digging and made 2 other discoveries:
- Gluten is not necessarily to blame because FODMAPs cause problems. Because bread can be high in both FODMAPs and gluten, somebody may mistakenly believe that gluten is the problem when it may actually be the FODMAPs. The Monash University website has a great webpage where they explain their perspective on gluten, FODMAPs, and non-celiac gluten sensitivity. In practice, a low-FODMAP diet is very annoying and people don’t like sticking to it. So let’s get to the next discovery…
- Hypnotherapy is highly effective for treating IBS. See this webpage on the Monash University website. Another way of looking at this is that the gluten-free diet has strong placebo effects and that you can get the same benefit through hypnotherapy without having to put up with the inconvenience of eating gluten-free.
So if a gluten-free diet is helping with your IBS, you can look into these alternative theories because they may be more convenient or they may give you better health outcomes. And of course your medical team should rule out celiac disease because it can cause IBS-like symptoms.
Autoimmune disease
There are scattered case reports of gluten-free diets reversing autoimmune disease. The chance of this happening seems to be low. See the following post for a deeper dive:
How-to Guide
See the post below for a newbie’s guide on how to get started.
There is a harder version of the gluten-free diet for people who may be extremely sensitive to very small / trace amounts of gluten.
Closing thoughts
Yesterday, I began highlighting a safe-ish treatment (avoiding exercise) for people who have been beaten down by treatment going badly. This post continues that theme. The survey data suggests that a gluten-free diet is even safer than avoiding exercise.
As far as the benefits go, it’s unclear if this diet will help treat the underlying cause of vaccine injury. However, patients really like this treatment (on average). According to the survey data from April 9, 2023… this diet is the #6 treatment among the 56 most popular treatments (*this is among ALL participants, not just the people who are mostly recovered).
So why not think about whether or not gluten-free is for you? This may be something that you knead in your life.