My thoughts on the Swedish HBOT study (Anders Kjellberg and colleagues)
Recap of the study results
Anders Kjellberg and his colleagues conducted a RCT on Long COVID patients (NCT04842448). The study compared high pressure HBOT at 2.4bar with 100% oxygen to a sham/‘placebo’ treatment (going from 1.34 to 1.2 bar HBOT; with placebo medical air).
Both the placebo (low pressure HBOT) group and treatment group improved over time.
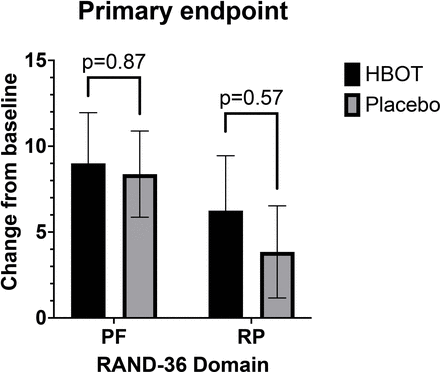
While the treatment group had slightly higher improvement as measured by RAND-36 scores (for Physical Functioning and physical health), the difference was not statistically significant. A larger trial with 260 patients (130 in treatment and 130 in control) could, in theory, yield statistically significant results if there is an underlying benefit to HBOT.
The trial also measured patient outcomes via the 6 minute walk test, reactive hyperaemia index, 30-second chair-stand test, EQ-5D-5L index, and EQ-5D VAS. The results on these secondary endpoints was not statistically significant (see Table 2 in their paper). For all 5 secondary endpoints, the placebo group improved slightly more than the treatment group (!).
The results not being statistically significant; results conflict with the Israeli study
The sham treatment in the Israeli Shamir Medical Center study went from 1.2 to 1.03 ATA.
The sham treatment in the Swedish study went from 1.34 to 1.2 bar, which is ~1.32 ATA to ~1.18 ATA.
So, the Swedish sham treatment is vaguely similar to low pressure HBOT (which can be achieved with cheaper soft shell chambers). That could explain why the sham group in the Israeli study saw little improvement while the sham group in the Swedish study saw a lot of improvement.
That the sham group in the Swedish study got better is interesting. I always thought that low pressure HBOT does very little and that you need high pressure HBOT to get results (because that’s what my survey data indicated/suggested). I… don’t know what to think anymore.
If you dig a little deeper into the Swedish data, the secondary endpoints suggest that the sham group improved more than the treatment group (!). That result doesn’t make a lot of sense.
Placebo effect, low pressure HBOT doing work, or reporting biases?
The sham group actually did get better (on average). (There are probably people who got worse and many people in the sham group who discontinued treatment.)
I personally doubt that there’s a placebo effect in long COVID. The condition doesn’t look like IBS where hypnosis was a highly effective treatment in this RCT study. Long COVID doesn’t magically go away after meditation, acupuncture, trying lots of treatments, etc. etc.
The study could be measuring reporting biases. People answer questionnaires and surveys in weird ways. For example, some people will start ‘speedrunning’ surveys if it is very long or if they are subjected to an extensive amount of medical testing and questionnaires (the Swedish study did that). The subjects had to take the same survey 5 times. There’s weird-looking data such as the responder rates over time (as measured by the PF and RP portions of the RAND-36 questionnaire). For the HBOT group, it consistently went up according to PF - but it whipsawed around according to RP.
It may also be the case that low pressure HBOT does something. That would be very interesting if true because cost won’t be such a huge barrier.
The Swedish researchers’ thoughts
The paper talks about (theoretically) doing a study with more patients. It also talks about giving patients more HBOT, in line with the Israeli study. In the conclusion of the paper, the authors lean into the idea that they didn’t HBOT hard enough.
Further studies with subgroups for male and female populations and a dose of more than 10 sessions are required.
Safety of HBOT- both low and high pressure
In the Swedish study, 15% (6/39) in the HBOT treatment group discontinued while 7% of the sham group (3/41) discontinued. There was a severe adverse event in the treatment group and a suspected suicide in the sham group.
The paper nonetheless states:
HBOT delivered with medical grade oxygen and hospital standards of chamber safety seems safe for previously healthy patients with long covid.
The paper also acknowledges that the ‘sham’ treatment (when went from went from ~1.32 ATA to ~1.18 ATA) is sufficient stress for the patients to have a
physiological effect, which may explain the:
- Unexpectedly small difference between active treatment and
sham treatment - The similarities in AEs
I would argue that both groups got at least a little bit of HBOT. Survey data on low-pressure HBOT suggests that low pressures are enough to cause patients to report negative experiences. It’s suggestive of low pressure HBOT doing work- good in some patients and bad in others.
The Swedish study paper discusses its safety findings versus the Israeli study:
Previously published RCT reported no significant difference in side effects between the groups (35.1% and 38.9%, p = 0.739 in the HBOT and control groups, respectively) and no discontinuation of the treatment due to side effects.10 Most previous trials with HBOT have not reported AEs in compliance with ICH-GCP.35 The similarities in AE occurrence between groups suggest that the AEs are not related to oxygen itself. Given the frailty of this group, it’s possible that AEs occurred in the placebo group due to the effort of participation, by breathing non-humidified air in sham treatment or would be observed in those subjects even without treatment. There is also a possibility that the sham treatment is sufficient stress for this group of patients to have a physiological effect, which may explain the unexpectedly small difference between active treatment and sham treatment, and the similarities in AEs. Alternative explanations for the higher rate of AEs are difference in disease severity, difference in treatment protocols (2.0 ATA vs 2.4 ATA) or differences in reporting of AEs. Our trial was conducted in compliance with ICH-GCP, which includes a meticulous reporting of AEs.
Disclosure / my bias
My bias is that I want HBOT to be helpful. If it isn’t, then patients just have to accept their crippling health problems and hope that they are among the people who are lucky enough to spontaneously recover.
Final thoughts
The results of this study are disappointing because we don’t have a clearcut answer as to whether or not HBOT is helpful.
If it is helpful, it is only helpful for a minority of patients. Response rates are low.
As far as finding effective treatment for Long COVID goes, here are my thoughts:
- Measuring patient outcomes is hard. Studies can easily measure things that aren’t health outcomes.
- Patients have tried almost everything.
- If patients have found effective treatments, treatment response rates are very low (perhaps a few percent). This makes Long COVID expensive to study because we need big studies to find weak signals.
- The endgame may be finding more treatments with very low response rates. We’re just going to have to find a lot of them.
It’s going to be a long road.
In other news, I consider myself fully recovered now (instead of mostly recovered)… and I’ve never done HBOT. The challenge is to figure out recovery for everybody… because copying what I did won’t work for the vast majority of people. ![]()