Data on Long COVID and dental implants
A case study series described by Michael Block (DOI:10.1016/j.joms.2021.01.033) suggests that dental implant failures are more common among patients who have previously had COVID-19 and are more common soon after developing COVID.
Data on COVID vaccines and fillers
There is a case report by Alain Michon (PMID:34174156) about two patients reacting to a hyaluronic acid soft tissue filler.
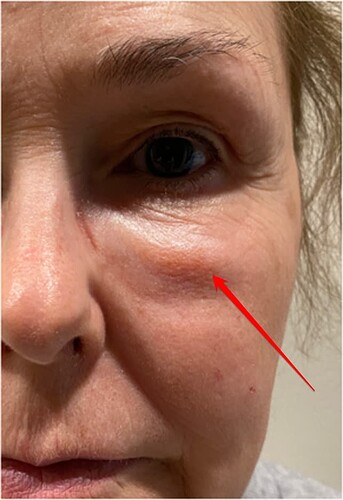
A 39-year old female who previously had her tear trough area treated with hyaluronic acid soft tissue filler developed swelling days after getting the mRNA Pfizer-BioNTech COVID-19 vaccine. Another patient, a 61-year-olf female, developed intermittent facial swelling in areas previously treated with hyaluronic acid soft tissue fillers days after receiving her first dose of the mRNA Pfizer-BioNTech COVID-19 vaccine.
[…]
Delayed inflammatory reactions to hyaluronic acid soft tissue fillers are uncommon and usually self-limited, with frequent spontaneous resolution. However, considering the ongoing pandemic and the worldwide demand for vaccines against COVID-19, the aesthetic providers should be conscious of the risks posed by the interaction of such vaccines in patients who previously had or seeking hyaluronic acid soft tissue filler injections.
We don’t have extensive or highly reliable on cosmetic fillers in Long COVID patients. You do run the risk of having an unpleasant experience.
The fillers do leave your body over time so it’s possible that the side effects will not persist after that. However, we do know from Breast Implant Illness patients that many people have lingering symptoms even after the removal of their breast implants. So, while most people respond positively to removal/explantation, we shouldn’t just assume that there will not be any long-term side effects.
I may be the only weirdo in the world trying to collect data on this stuff. We may not get a good, satisfying answer about the exact risks of various foreign objects in long haulers. However, there is reason to be concerned.
Botox, Dysport, etc.
Botox contains botulinum toxin, which is a nerve toxin. The word toxin is literally in the name of Botox’s active ingredient (e.g. Clostridium botulinum type A neurotoxin complex). In some patients, Botox injections are known to spread outside of the targeted area and cause nerve damage. The treatment/procedure now carries a Black Box warning to highlight that phenomenon.
WARNING: DISTANT SPREAD OF TOXIN EFFECT
See full prescribing information for complete boxed warning.
The effects of BOTOX and all botulinum toxin products may spread from the area of injection to produce symptoms consistent with botulinum toxin effects. These symptoms have been reported hours to weeks after injection. Swallowing and breathing difficulties can be life threatening and there have been reports of death. The risk of symptoms is probably greatest in children treated for spasticity but symptoms can also occur in adults, particularly in those patients who have an underlying condition that would predispose them to these symptoms. (5.2)https://www.accessdata.fda.gov/drugsatfda_docs/label/2011/103000s5232lbl.pdf
There are various scientific papers on “iatrogenic botulism”, which is another way of saying that a medical procedure gone wrong gave you botulism (botulinum toxin poisoning).
We do know that many (but not all) long haulers have problems with their autonomic nervous system or some form of dysautonomia. Neurotoxins are known to cause problems with the autonomic nervous system.
If you already have dysautonomia, maybe it’s not a great idea to layer on a neurotoxin on top of that.
Recap
Usually these products are used for cosmetic purposes and can be avoided. So, you can simply find alternatives that are safer or less risky. There are other things that you can do with your money.
Appendix
Science primer
Potential mechanism of foreign body adverse reactions - fungi and bacterial biofilms
In many areas of the scientific literature, it is well-established that fungi and bacteria can grow on foreign objects in the body such as replacement joints.
- A joint infection study by Achermann and colleagues (https://dx.doi.org/10.1128%2FJCM.00006-10) have found Staphylococcus aureus, Coagulase-negative staphylococci, Streptococcus species (mitis, agalactiae, dysgalactiae, gallolyticus, pneumoniae), Propionibacterium acnes, and Candida albicans.
- Koskela and colleagues (Prevalence of the ica operon and insertion sequence IS256 among Staphylococcus epidermidis prosthetic joint infection isolates | European Journal of Clinical Microbiology & Infectious Diseases | Springer Nature Link) as well as Hischebeth and colleagues (Redirecting) discuss the role of Staphylococcus epidermidis in replacement joint infections.
Fungi and bacteria have also been found to grow on breast implants, though there is controversy as to whether or not Breast Implant Illness is real and if so, what is its cause.
- The study by Lee and colleagues (https://dx.doi.org/10.1097%2FGOX.0000000000002755) found that Propionibacterium acnes , Staphylococcus epidermidis , and fungal Candida species all grow on implants.
Survey data from the Risk Factors survey suggests that both replacement joints and breast implants are risk factors for Long COVID and post-vaccination syndrome.
There are also case reports of vaccine reactions related to breast implants:
- Potential immune response to breast implants after immunization with COVID-19 vaccines Redirecting - Case series on 4 patients
- Breast implant seroma: A SARS-CoV-2 mRNA vaccine side effect https://doi.org/10.1002/jcu.23056 - Case study
- A Case Report of Capsular Contracture Immediately Following COVID-19 Vaccination https://doi.org/10.1093/asjof/ojab021
Fungal and bacterial biofilms could potentially explain why long haulers react to facial fillers.